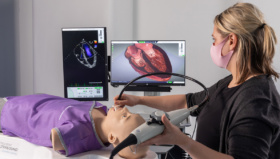
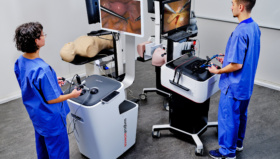
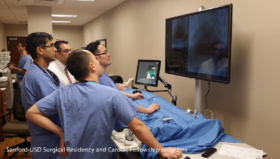
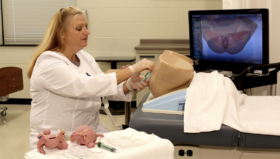
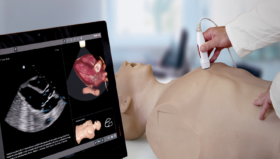
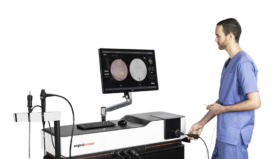
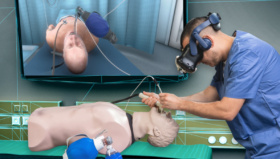
VR Simulation and Accelerating the Learning Curve
We talk with a top UK surgeon on surgical training and long learning curves, and how VR simulation can help improve surgical training.
You can also download our whitepaper – Learning curves and the costs to surgical training – and learn how VR simulation is changing the shape of surgical training with regards to patient outcomes, patient safety and cost-efficiency.
 Wyn Lewis is a consultant general surgeon and professor at Cardiff University, Wales, with an education role as the head of school of surgery for Health Improvement Wales.
Wyn Lewis is a consultant general surgeon and professor at Cardiff University, Wales, with an education role as the head of school of surgery for Health Improvement Wales.
Over the past few years, Wyn has published several papers on learning curves in surgical trainees and how VR simulation affects learning curve trajectories.
Hi Wyn. Could you briefly explain learning curves and how it relates to surgical training?
There are a lot of misunderstandings about learning curves, politicians talk about something that is difficult has a steep learning curve. In fact, if a learning curve is steep, then you hit competence very quicky. So, a steep learning curve equates to an easy procedure not a difficult procedure. A difficult procedure, the curve is very gradual and that is a big misunderstanding.
Do you think VR simulation can have an impact on the surgical training learning curve?
Yes, it can. It can get certain people up the learning curve quicker, and with simulation there is no risk to any patients involved. The other benefit is the better use of trainer time. If you have got a trainee 80% of the way to the inflection point when they are competent, then that is much better use of a trainer’s time than have them focusing on the first 20 % of the learning curve.
You can also focus on the more difficult challenging parts of a procedure. For example, not all appendicectomies are easy, some are very straight forward, you can then focus on how get yourself out of trouble with more challenging situations when you have a difficult appendicectomy. And that applies to all operations.
In your recent paper Operative Learning Curve Trajectory in a Cohort of Surgical Trainees, you discusses the issues of surgery training in the UK. What were the circumstances that lead to the writing of this paper?
In the UK, our general surgery curriculum is set by the Joint Committee on Surgical Training (JCST). And we have six indicative operations that every general surgeon must prove to be competent in, and the most common emergency operation is appendicectomy. The committee state that a trainee is required to do a minimum of eighty appendicectomies over six years to prove competency, but there is very little academic rigor as to where that figure comes from.
So, we wanted to investigate how many caseloads it took for a person to become competent to do an appendicectomy. And the number, after looking at 60 trainees, was 95 procedures. And we thought this was a very high number to us, we thought it should be closer to 20.
95 cases is a very high caseload. The data for median number caseloads for a cholecystectomy, is also high, 87, and you state that it can take up to 4 years for a trainee to become competent in both these procedures.
Yes. Cholecystectomy is a more challenging procedure. To operate and remove a patient’s gallbladder involves appreciation of more complex and may prove to be anomalous anatomical variations. An operative error in that field can result in catastrophic consequences, which may be life threatening. Which is why it takes longer.
And do you think there is a more efficient way of training in surgery? And is VR simulation the solution to that?
Simulation is part of the answer, there is no getting away from the fact that trainees would prefer to train on actual patients, and you can train on cadaveric tissue now, very realistically, but the cost of that is way beyond the cost of VR for example.
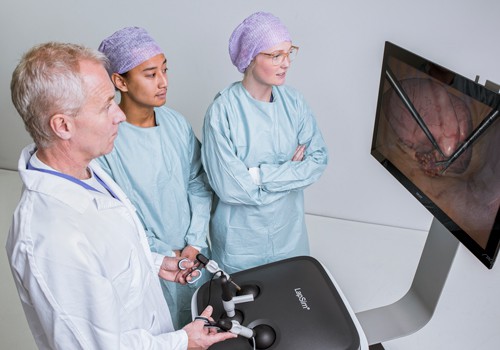
And how do you think this has an impact on patient outcomes?
The more efficiently and the quicker the procedure is done, without complications, the better the patient outcomes should be. Then the patient can be discharged early, often the next day. At present durations of hospital stay vary considerably, often at significant extra cost. And the less experience they have [trainees] the longer the procedure will take. And that’s understandable because they fear making mistakes.
And do you think VR simulation can help students gain more experience?
Yes. Also, with a LapSim simulator you can raise the difficulties for each procedure, program in that the appendix will perforate and how you deal with that. A trainee will maybe do 50 appendicectomies over a course of 3 years but they may never see retro-caecal appendix [where the appendix is hidden behind the caecum]
Do you think most surgeons are onboard with VR simulation training?
I think there is a great deal of ignorance , people are unaware of it. And the speed at which it is developing. I only know about your company because you happen to be in the next room when we were running a course and I saw your EndoSim and I was so impressed at how close to reality developments had reached.
Was that important?
Yes, the more realistic it is the easier it is to get trainers and trainees to buy into it.
And from what you’ve seen so far, do you think your residents are enjoying VR simulation training?
There are limitations but absolutely, they were very grateful for the simulation training we gave them.
And with LapSim simulation?
With LapSim you can review you own performance and play the video back, the trainees did comment that that was a particular useful feature.
Going back to ethical implications and learning curves. Instead of training a residents’ first 20 caseloads on patients you could train with VR simulation. Do you think it is common knowledge that patients are being used to train on at this very early stage of resident training?
This is the way that training has always been done; the apprenticeship model. It is common sense that if you have done 10 virtual procedures, that the first live case, should be easier and better. The left shift of the learning curve. You reach the inflection point of the learning curve and competent level quicker.
A good example I use about this, is flight simulators. It’s embedded in the airline industry, proving yourself on a simulator.
I think if you knew that your surgeon had done x amount of training on a simulator they would feel more comfortable and less worried about their operation.
Absolutely.
So you think there is a real future for VR simulation training.
Absolutely, if we had the financial resource, we’d have these LapSim and EndoSim simulators in every training unit. But where would we put them? Moving forward we could move them to safe areas, outside of hospitals, so they are readily accessible to the trainees.
I think we need a number of core simulation centers where you could book in trainees for a few weeks and put them through the modules. We don’t have a dedicated simulation centre in Wales, though there is a will to do that and it would require a lot of financial investment. But that investment would arguably pay for itself within 4 or 5 years, as you could in theory reduce training time significantly.
If we had enough VR trainers, we could make sure that surgeons are at a certain level, a certification that they have a certain level of competence then you know where you are starting from.
Finally, any aspects of simulation you will be researching next?
It would be interesting to know what the outcomes are for appendicectomies with the units that have LapSim, we’re not in a position to do that right now with LapSim but we are with EndoSim.
We put 28 trainees through, 18 months ago, it would be interesting to look at whether or not that the 28 people that went through, had achieved their JTS competences quicker than their peers who did not go through. And that will be the next part of the research whether they achieved their three level 4 competence quicker than their peers.