Poland Leading the Way in Simulation Training
 Poland is the first country in Europe to have created a national assessment program for all endoscopic and laparoscopic surgical procedures.
Poland is the first country in Europe to have created a national assessment program for all endoscopic and laparoscopic surgical procedures.
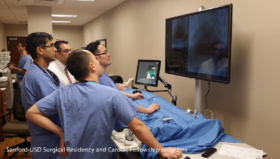
Many medical training facilities around the world are slowly shifting from the traditional ‘apprenticeship’ method of education to ‘simulation and examination’ models that remove patients from the initial learning phase in procedural training.
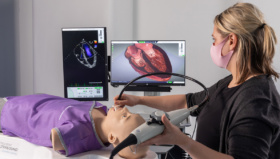
Professor Michał Pirożyński is Head of Endoscopic Simulation at the Center for Postgraduate Medical Education (CMKP) in Warsaw, Poland. His postgraduate course in bronchoscopy was one of the first to introduce a mandatory program of simulation training, meaning that all trainees must demonstrate a certified level of proficiency before coming into contact with patients.
“The apprenticeship model is insufficient when it comes to performing bronchoscopies on critically ill patients with acute respiratory problems,” Prof. Pirożyński says. “Not only is it clinically unjustified, it is also unethical. These are people, not guinea pigs. And yet many training facilities still employ the old Halsted model of education: ‘see one, do one, teach one’. For many years, my colleagues and I have been developing simulation training techniques that make bronchoscopies safer and more effective.”
Prof Pirożyński has performed thousands of bronchoscopies over a career spanning more than 50 years. During that time, he has seen huge advances in surgical techniques and equipment. In the early days, bronchoscopies were performed using rigid metal scopes that were inserted into a patient’s airway. Often, these procedures were done under local anesthetic, meaning patients were conscious throughout. Trainees were provided with a mentor, and they learned ‘on the job’.
“I vividly remember the first time I performed a bronchoscopy on my own,” Prof Pirożyński recalls. “The patient was a 78-year-old woman and she needed fluid draining from her airway. I was terrified, but I had two things in my flavor: Firstly, the patient had experienced the procedure before, and, second, she had no teeth, so it was much easier to insert the scope! In the end, she was much more relaxed than I was, but I realized from that moment that the apprenticeship model was not sustainable. There had to be a better way.”
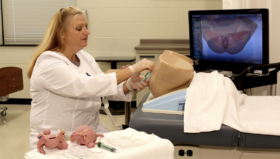
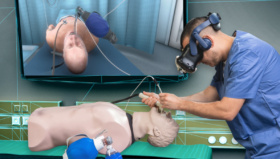
For Prof Pirożyński, using simulation to replace supervised procedures on patients became an essential part of teaching bronchoscopies. Not only did it allow trainees to practice over and again in a safe environment, it removed the psychological burden of working on sick volunteers. The problem was in developing simulation tools that best reflected the ‘real world’ surgical experience.
A big breakthrough came with the advent of fiberscopic tubes which were flexible and less invasive for the patient, but they added complexity as trainees had to learn how to control them effectively.
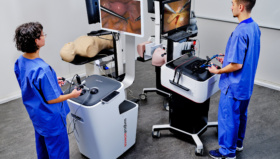
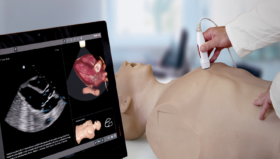
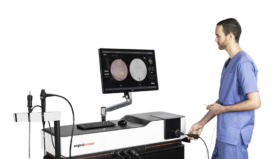
I am a big believer in visualizing the training experience,” Prof Pirożyński says. “I always encourage trainees to try to imagine how their instruments feel as they maneuver them around the body. Of course, you have to know your anatomy, but you also have to repeat the task again and again until it becomes second nature. The early simulation tools we used were quite crude – we designed models of a patient’s trachea using papier mâché! – but now we have extremely sophisticated 3D simulators that allow trainees to see exactly what is happening. They can even simulate the resistance users feel against their instruments. It is a truly immersive experience.
Today, the Polish National Assessment Program is recognized internationally as a gold standard in postgraduate training. All trainees in endoscopy and laparoscopy are required to complete a six-day course, which is split over two periods weeks apart to ensure the knowledge is retained. There are then standard examinations which must be passed before a trainee can set foot inside an operating theatre.
Prof Pirożyński believes simulation should be the standard tool for medical training everywhere. “We have been lucky in Poland as we have a single, centralized postgraduate training facility, so we can shape a training program that provides continuity across multiple surgical disciplines. We believe our framework helps to better prepare postgraduates for performing all types of procedures. If it can be replicated in other countries, that will produce more confident, competent medical professionals and better patient outcomes.”
The initiative described in this article is funded by the EU program: ‘Development of specialty training of physicians in the use of endoscopic techniques using simulation, in fields relevant to the epidemiological and demographic needs of the country’ (UDA-POWR. 04.0300=00-0291/16-00)