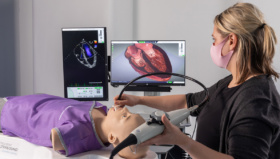
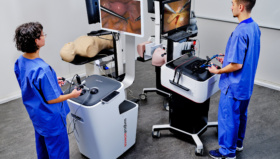
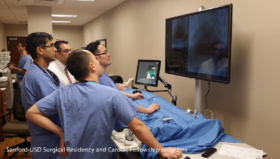
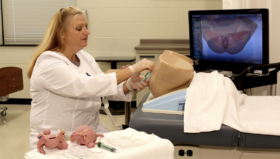
In Denmark, physicians undergoing training in vascular surgery must pass a simulation exam before they are allowed to operate on patients. That’s the only right thing to do, says the chief physician at Rigshospitalet hospital.

Before a future vascular surgery surgeon in Denmark can be allowed to operate on patients with poor circulation in the legs, the physician must pass a series of advanced simulation exams.
Dr. Jonas Eiberg, chief physician at the Vascular Surgery Department at Rigshospitalet, said, “Our residents simply must not be involved in ballooning and stenting patients before they have passed the exam.”
Dr. Eiberg, is also a clinical associate professor with responsibility for the education of vascular surgeons in eastern Denmark. Dr. Eiberg explains that there is a requirement from the authorities that all residents must go through simulation training during their vascular surgery training.
“At Rigshospitalet, we have taken it a step further. Our vascular surgeons residents simply do not come close to patients until completing simulation training and all exams. That order is the only one that makes sense,” he says.
“We have started practicing simulated endovascular balloon and stent interventions, but the future lies open. There are many other vascular surgeries where simulation training can and should be implemented – first and foremost for the sake of patient safety,” said Dr. Eiberg.
An opportunity to make mistakes
The background for the new virtual exams is that new minimal invasive techniques using balloon and stent have replaced many classic open vascular surgeries.
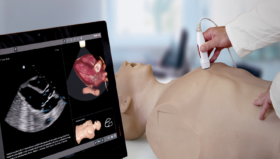
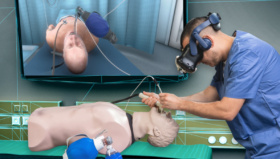
“The new technology is very technical. The surgeon must be introduced to a whole new toolbox with balloon catheters, sheaths, guidewires, stents and endografts. Simultaneously, the surgeon must operate and understand advanced x-ray equipment. Studies have shown that balloon and stent interventions present ample opportunities to make mistakes. The consequences of the errors are often significant and difficult to correct, “says Jonas Eiberg. “With the old-fashioned educational strategy, the so-called peer education, there is a high probability of making mistakes which could have been avoided, because we have traditionally started by practicing on patients. Simulation training provides the opportunity to train demanding, new operations in a zero-risk environment for the patient,” he says.
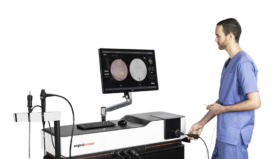
“They made all of their mistakes on the simulator,” said PhD student and physician, Jonathan Lawaetz Rasmussen who is in charge of leading future specialists in vascular surgery through three simulation modules, each with a dedicated exam. “They have to complete three modules with me during the program. Each module is focused on an underlying disease, so that they get trained on the most important techniques. Physicians must pass module one before proceeding to module two and so on. They are allowed to practice as many simulation sessions as they want until they pass twice in a row. Only at this point we are certain that they acquired the necessary skills. They do not get the course approved until they are proficient enough.”
Dr. Jonathan Lawaetz Rasmussen is writing his Ph.D. on simulation-based training of vascular surgeons and is affiliated with the Vascular Surgery Department at Rigshospitalet, as well as CAMES, an education and simulation center in the capital region, under the guidance of Dr. Eiberg.
Are there any participants who do not pass the three exams?
“There is a big difference between people. There’s someone flying through, and then there’s someone that keeps trying again and again.” said Jonathan Lawaetz Rasmussen.
Researchers from the University Hospital in Ghent have developed the program, PROSPECT (PROficiency BasedStePwise Endovascular Curricular Training) used in Rigshospitalet. Jonathan Lawaetz Rasmussen works with the research team in Belgium.
“Our colleagues in Ghent have shown that the cases where the supervisor intervenes and takes over the operation – what is called supervisor takeover – decreases significantly if its resident went through simulation training,” said Jonathan Lawaetz Rasmussen. Randomized trials have shown that physicians who were trained by the program are more skilled.
“They have made all their mistakes on the simulator. The sideman training could not match the simulation training,” said Dr. Jonathan Lawaetz Rasmussen.
Together with the researchers in Ghent, he is in the process of further developing the program. He examines, among other things, how future vascular surgeons can best and most quickly learn important skills.
Nurses also participate
It is not only the future vascular surgeons at Rigshospitalet who gets the opportunity to pass simulation exams. On his initiative, in the vascular surgery department at Rigshospitalet involved the vascular surgical nurses, who assist in balloon and stent interventions, in the training on the simulator.
“All the nurses review the theory, practice balloon dilation and stent deployment on the simulator – they go through a program which is similar to the physicians’,” said Dr. Jonathan Lawaetz Rasmussen. “Although the nurses do not have to perform the procedure themselves, the simulation training provides a completely different understanding of the critical phases, the different steps of the procedure and the choice of equipment. It provides a better flow and understanding between the professional groups as well as fewer errors. This means that you are always at the forefront. The nurses have almost stood in line to attend the course, and the surgeons are very excited about this upgrade of assistance.” He also indicated that simulation-based training can better ensure the quality of the training course as you have to practice before cutting or puncturing the patients. “That is what the future holds.”
Original article:
https://dagensmedicin.dk/nye-krav-paa-riget-laeger-skal-bestaa-denne-test-for-at-operere/