The COVID-19 pandemic has caused many issues in healthcare over the last 18 months. For many surgeons and medical professionals, it has had led to time away from normal medical practise. This means they have been unable to perform their regular medical, surgical or robot-assisted tasks. In turn, this has led to problems such as skill decay, where competences, such as surgical skills, decline over a period of time due to their lack of use. Skill decay in surgeons raises concerns for patient safety and patient outcomes. In this article we look at the implications of skill decay and how the regular use of a virtual reality (VR) simulators can help reduce it.
Inactivity Due to Covid-19
During Covid-19 many surgeons were obliged to work in environments away from their field of expertise and have not been able to perform specific surgical procedures for an extended period of time due to other work commitments (Hedman, 2020).
In the UK, according to the Joint Committee on Surgical Training, there have been over 900 thousand elective surgeries that have been postponed or cancelled due to the pandemic, which has also meant that surgical residents have not been able to train in all surgical procedures.
Worldwide, an estimated 82% of benign surgeries, 38% of cancer surgeries, and 25% of elective caesarean sections were cancelled or postponed during the 12-week peak of COVID-19 alone (British Journal of Surgery, 2020).
These factors mean that for the last 18 months surgeons and other medical professionals have not been able to perform their normal jobs, which has major implications, particularly in terms of skill decay.
The Impact of Skill Decay
Skill decay is the partial or full loss of acquired skills and knowledge following time away from practise. For example, acquired surgical skills can be prone to decay, especially after a long period during which they are not practised, and can degrade in as little as 2 weeks (Kelc 2020).
Skill decay can be more apparent in difficult medical skills such as laparoscopy. For example, a paper presented at Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) on Expert surgeons’ skills decay in simulated laparoscopic surgery: the relevance of task difficulty stated that “High risk difficulty maybe with greater potential for skill loss in clinically expert laparoscopic surgeons” (Ruchi Thanawala, 2011).
Furthermore, certain aspects of complex skills can decline more than others, as reported in Hardie (2020). “After one-year away from surgery for research, trainees perceived a larger decline in complex technical skills, such as bowel anastomosis, than for more routine operations such as hernia repairs. Six months following laparoscopic training, instrument and tissue-handling skills deteriorated more than speed, particularly fine motor skills. In addition to technical skills reduction, trainees taking time out for research also perceived a reduction in their clinical judgment.”
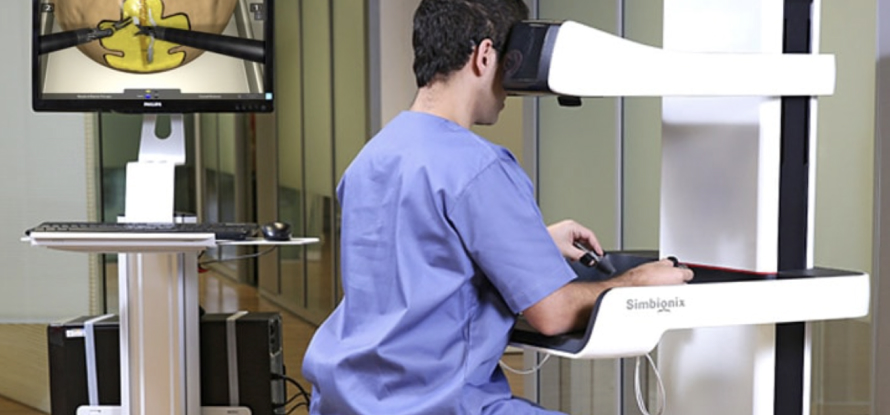
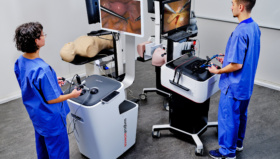
Skill decay also affects robot assisted surgical skills, which can degrade rapidly – within 4 weeks of inactivity in newly trained surgeons, according to one study (Jenison, E. L, 2012). It is important it for surgeons to maintain their robot assisted surgical skills during a period of inactivity.
Additionally, skill decay in a surgeon can lengthen the time of an operation, even after relatively short periods of inactivity. Sugihara 2018, for example, showed that an absence of less than 15 days can have an adverse effect on the length of an operation.
The decline of technical expertise and even decision-making skills can have a large impact and is a matter of concern in terms of patient safety, patient outcomes and potential medical errors.
The Need for VR Simulation Training
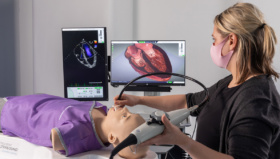
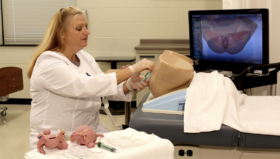
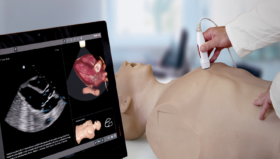
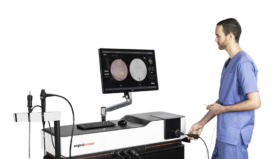
VR Simulators, such as the LapSim simulator, are now considered to be an invaluable tool for surgical training (Larsen, 2009) and can also be used to maintain surgical skills for residents and experienced surgeons.
Practise on simulators, especially during long periods of inactivity, means key competences such as psychometric skills can be retained, allowing surgeons to be well-prepared before performing on real patients.
An article from Surgical Innovation showed that proficiency-based simulator training results in durable improvement in operative skill of trainees even in the absence of practice for up to five months (Stefanidis, 2008).
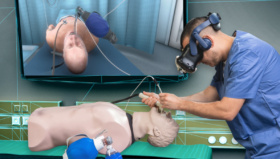
An increase in opportunities for VR simulated surgical training can help residents and experienced professionals retain basic competence. One way to keep skills acquisition and prevent skill decay is to provide increased possibilities to practice simulated surgical tasks, i.e., psychomotor training including virtual training (Hedman 2020). “When used appropriately, extended simulation training can be a highly effective additional training tool in the development and maintenance of technical skills and combatting skills decay. This is relevant also for temporarily non-performing orthopedic surgeons during a crisis affecting the organization of healthcare such as the COVID-19 pandemic” (Hedman 2020).
In the absence of elective surgeries that have either been postponed or cancelled surgical VR simulation is a powerful tool that can help meet training demands (Leif Rune, 2020). Kogan et al. (2020) made clear that isolation away from patient care, active social distancing, and a fall in case volume during the pandemic will increase the need for surgical simulation training.
Referenses
British Journal of Surgery, Volume 107, Issue 11, October 2020, Pages 1440–1449, https://doi.org/10.1002/bjs.11746, accessed 10 November 2021
Hardie JA, Brennan PA. Are you surgically current? Lessons from aviation for returning to non-urgent surgery following COVID-19. Br J Oral Maxillofac Surg. 2020 Sep;58(7):843-847. doi: 10.1016/j.bjoms.2020.06.012. Epub 2020 Jun 19. PMID: 32576468; PMCID: PMC7303632
Jenison, E. L., Gil, K. M., Lendvay, T. S., & Guy, M. S. (2012). Robotic Surgical Skills: Acquisition, Maintenance, and Degradation. JSLS : Journal of the Society of Laparoendoscopic Surgeons, 16(2), 218–228. doi:10.4293/108680812×13427982376185
Larsen, C. R., Soerensen, J. L., Grantcharov, T. P., Dalsgaard, T., Schouenborg, L., Ottosen, C., Schroeder, T. V., & Ottesen, B. S. (2009). Effect of virtual reality training on laparoscopic surgery: randomised controlled trial, Larsen Christian R, Soerensen Jette L, Grantcharov Teodor P, Dalsgaard Torur, Schouenborg Lars, Ottosen Christian et al BMJ 2009; 338 :b1802.
Kogan M, Klein S E, Hannon C P, Nolte M T. Orthopaedic education during the COVID-19 pandemic. J Am Acad Orthop Surg 2020. doi: 10.5435/ JAAOS-D-20-00292. [Published online ahead of print May 7, 2020].
Hedman & Li Felländer-Tsai (2020) Simulation-based skills training in non-performing orthopedic surgeons: skills acquisition, motivation, and flow during the COVID-19 pandemic, Acta Orthopaedica, 91:5, 520-522, DOI: 10.1080/17453674.2020.1781413
Ruchi Thanawala, MD, Ron Bush, BS, Neal E Seymour, MD. Baystate Medical Center, Expert surgeons’ skills decay in simulated laparoscopic surgery: the relevance of task difficulty, accessed 20210, https://www.sages.org/meetings/annual-meeting/abstracts-archive/expert-surgeons-skills-decay-in-simulated-laparoscopic-surgery-the-relevance-of-task-difficulty/
Sugihara T, Yasunaga H, Matsui H, Ishikawa A, Fujimura T, Fukuhara H, Fushimi K, Homma Y, Kume H. A skill degradation in laparoscopic surgery after a long absence: assessment based on nephrectomy case. Mini-invasive Surg 2018;2:11 http://dx.doi.org/10.20517/2574-1225.2018.14
Stefanidis D, Acker C, Heniford BT. Proficiency-based laparoscopic simulator training leads to improved operating room skill that is resistant to decay. Surg Innov. 2008 Mar;15(1):69-73. doi: 10.1177/1553350608316683. Epub 2008 Apr 2. PMID: 18387999.