Step-By-Step to Proficiency
- User administration: create your training classes, and assign courses
- Curriculum design: pick from a pre-set library, and customize to your specific training needs
- Prepare for online learning: share videos and reading materials to participants before-hand
- Proficiency-based training: Perform the hands-on, goal-oriented, training
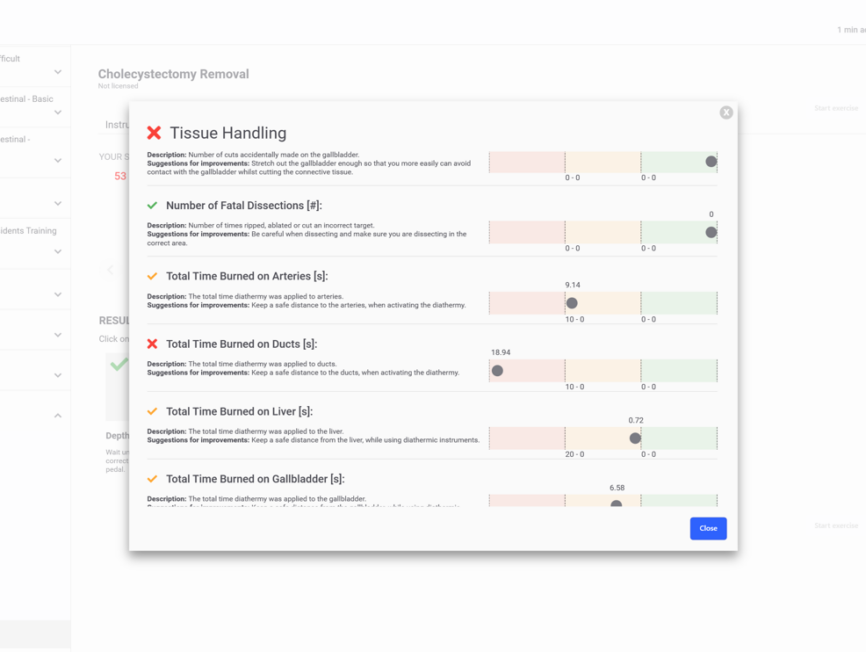
- Simulation debriefing: document participant progress with comprehensive objective metrics